blog
Sanator Series: The Importance of Provider Network Management
SECTIONS
In the evolving healthcare ecosystem, provider network management has emerged as a linchpin of optimal patient care, operational efficiency, and fiscal responsibility. Though sometimes overlooked, this facet of healthcare has overarching implications that touch every corner of patient care.
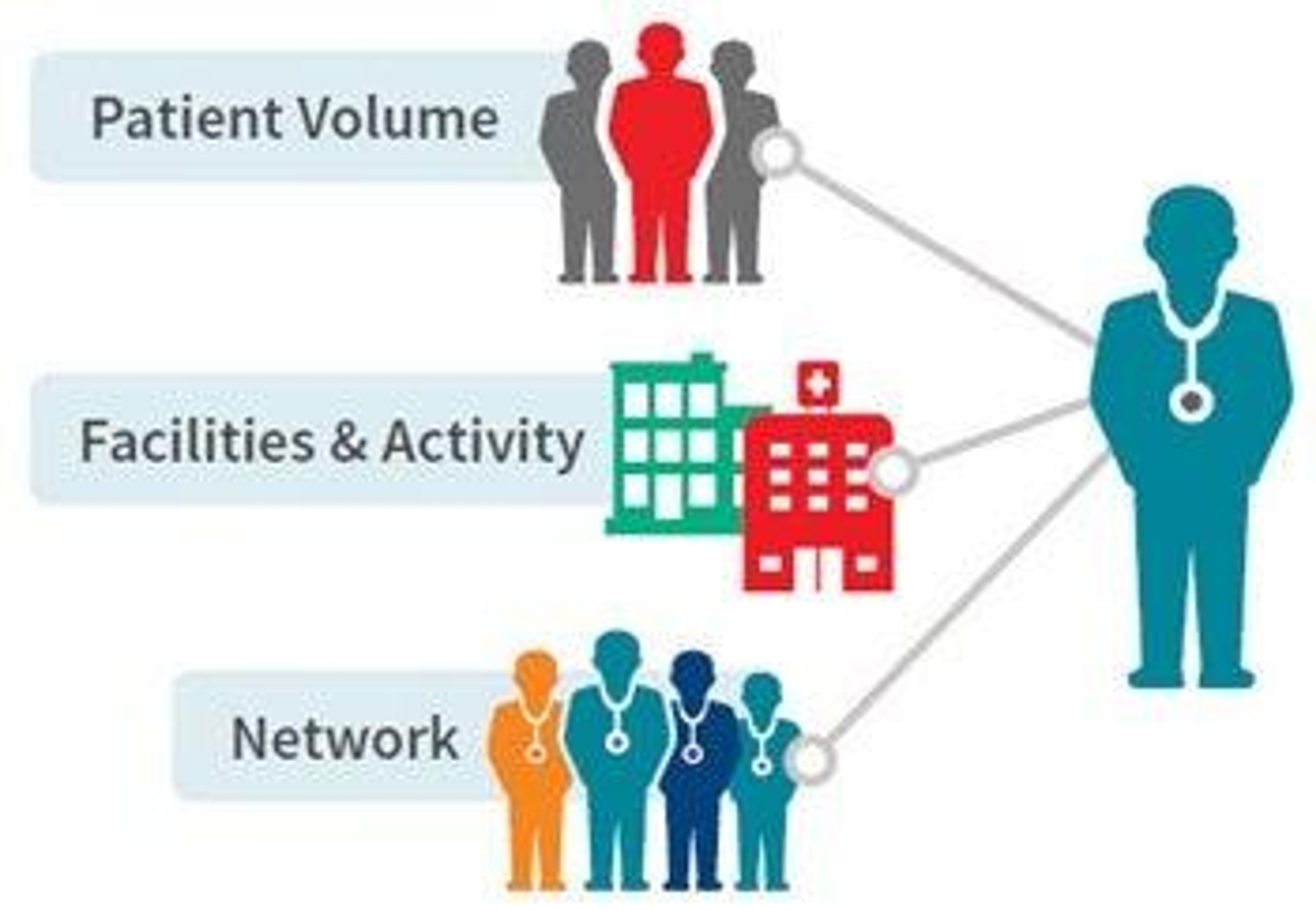
Image Source: risk.lexisnexis.com
1. Quality Assurance and Patient Safety
At the heart of provider network management is the assurance of care quality. Every provider, from generalists to specialists, needs to be vetted and credentialed. As noted by the Joint Commission, proper credentialing and privileging processes play a critical role in maintaining patient safety and care quality¹. Without rigorous network management, patients face increased risks of medical errors or inadequate care.
2. Economic Efficiency and Value-Based Care
As healthcare costs soar, the industry is shifting towards a value-based care model, emphasizing outcomes over volume. Provider network management is central to this transition. By eliminating inefficiencies and preventing over-utilization, a well-orchestrated network can offer significant cost savings while prioritizing patient needs.
¹ The Joint Commission. (2018). Credentialing and Privileging: Ensuring Competence. [Online]. Available at: Joint Commission’s official website.
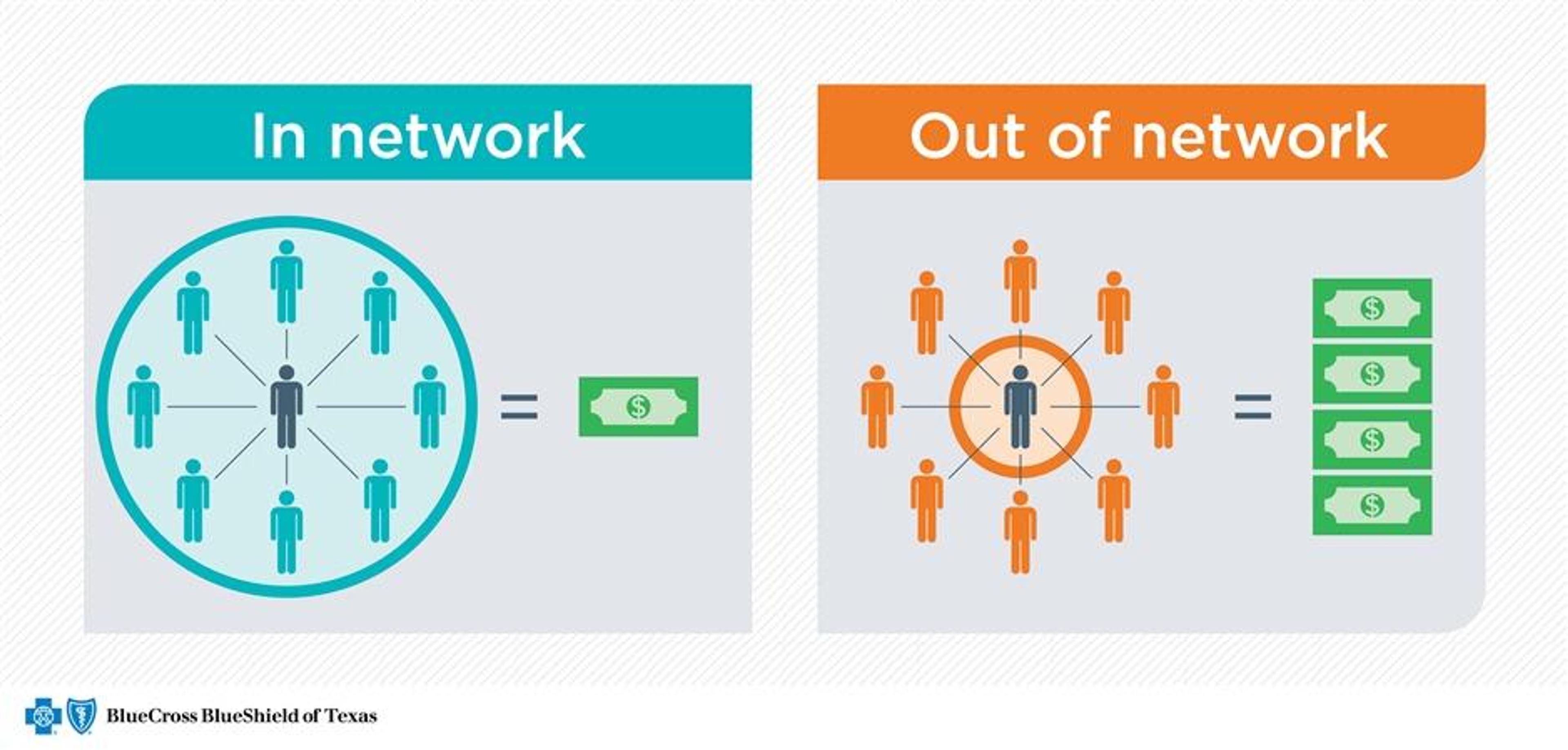
Image Source: connect.bcbstx.com
3. Elevating Patient Experience
Today’s patients demand both quality care and convenience. A study in the Journal of Medical Internet Research revealed that ease of access to care significantly affects patient satisfaction². Through efficient provider network management, patients can find and access the services they need promptly and conveniently.
4. Navigating Regulatory Compliance
The intricate web of healthcare regulations mandates a strict adherence to rules and standards. Comprehensive provider network management helps organizations remain compliant, sidestepping potential sanctions or litigation³. This protective layer ensures that patients receive care within a system that operates within established legal and ethical bounds.
5. Streamlining Collaboration and Coordination
Integrated care requires seamless collaboration across specialties. Provider network management acts as a bridge, ensuring smooth transitions and open channels of communication among providers. Especially for patients with intricate healthcare needs, this coordination is paramount for consistent and holistic treatment.
² Agarwal, R., Sands, D. Z., & Schneider, J. D. (2010). Quantifying the economic impact of communication inefficiencies in US hospitals. Journal of Medical Internet Research, 12(4).
³ Centers for Medicare & Medicaid Services. (2019). Regulatory Compliance and Guidance. [Online]. Available at: CMS’s official website.
Provider Network Management with Sanator by Gaine
In essence, provider network management is a cornerstone of a high-performing healthcare system. As the industry marches forward, the organizations that underscore its importance will undoubtedly stand at the forefront of quality care.
Learn how Sanator can help: https://www.gaine.com
